16, 17 Atomic force microscopy can achieve resolutions of 0.1Å and has the ability to measure immersed samples. By keeping the force constant, the tip remains at the same distance from the surface of the sample and thereby maps out the surface topography. This force is kept constant with a feedback mechanism that raises and lowers the cantilever by means of a piezoelectric element. A force on the order of piconewtons is created on the cantilever due to the proximity to the sample surface. Atomic force microscopy uses a sharp tip at the end of a flexible cantilever to scan and probe the sample surface. It was rapidly improved to enable operation in liquids, which made characterization of biological samples possible. 16 as a tool to investigate the topography of conductors and insulators on the atomic scale. 15 Atomic force microscopy was first developed by Binnig et al. 11 Atomic force microscopy (AFM) has also been used to image the corneal surface quality after photorefractive keratectomy 13, 14 and to quantify the smoothness of femtosecond laser cuts made in the posterior cornea at different laser energies. A profilometer based on the principle of 3-D confocal microscopy has been applied to the stromal surface to provide quantitative roughness information. To more accurately assess the smoothness of the stromal bed, however, it is vital to use a technique that provides numerical data of the surface topography.
Igor pro 6 mfp 3d bio manual software#
8, 9 This software produces a 3-dimensional (3-D) reconstruction of the sample surface based on differences in darkness of the grayscale images. However, using Scanning Probe Image Processor software (Image Metrology) to analyze the SEM images, quantitative surface roughness can be extracted. 2- 12 The smoothness of the cuts was determined qualitatively by visual inspection because SEM images alone cannot provide quantitative roughness information. The smoothness of the stromal bed after performing LASIK flaps and deep lamellar cuts (~400 μm) has been studied by several research groups using scanning electron microscopy (SEM). Several studies have assessed stromal smoothness after cutting with different femtosecond lasers to evaluate their efficacy. 2 Therefore, it is vital to quantitatively analyze the stromal cut quality produced using different lasers and settings as well as at different depths in the stroma. In LASIK and lamellar transplant surgeries (DSAEK and ALK), a smooth stromal surface will create a clearer interface, which in turn will produce better optical quality. In addition, the femtosecond laser is being used to prepare donor and recipient corneas for anterior lamellar keratoplasty (ALK) 1 and Descemet-stripping automated endothelial keratoplasty (DSAEK) procedures. This laser is also being used in lieu of traditional trephines for penetrating keratoplasty procedures.

Food and Drug Administration to create the flap during laser in situ keratomileusis (LASIK). The femtosecond laser is gaining popularity in the corneal refractive surgery arena, and multiple systems have been approved by the U.S.
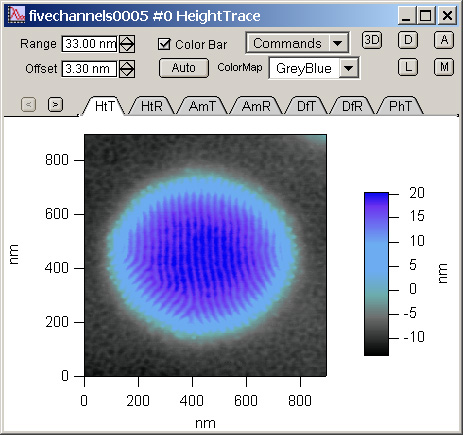
Four quantitative parameters (root-mean-square deviation, average deviation, skewness, kurtosis) were calculated from the AFM images. As a control, the posterior surface was placed in 2% formalin and imaged with environmental scanning electron microscopy (SEM). The anterior portion of the lamellar surface was placed in a balanced salt solution and imaged with AFM. A 12.0 mm trephination was then performed. The cut depths were 200 μm, 300 μm, and 400 μm, with the cut depth maintained for both eyes of each pair. The energy level was 180 nJ for the right eye and 340 nJ for the left eye of each pair. The eyes were placed in a holder, the epithelium was removed, and the eyes were cut with a Visumax femtosecond laser.

The eyes were reinflated to normal pressures by injecting a balanced salt solution into the vitreous cavity. The cornea was thinned to physiologic levels by placing the globe, cornea side down, in 25% dextran for 24 hours. Experiments were performed on 3 pairs of human cadaver eyes.
